
Episodic memory discrepancies seen in patients suffering from psychosis involve deficits in the medial temporal cortex, particularly the hippocampus, and in the PFC, particularly the ventral and dorsolateral regions (Brisch, 2014). Furthermore, increases in both phasic and tonic activity in the PFC, commonly seen in patients suffering from psychosis, leads to an increase in inhibitory post-synaptic currents, which would ultimately cause inhibition in the thalamus (Avery, 2017).
Neurochemical Abnormalities of Psychosis
Regarding the more direct neurochemical abnormalities of psychosis, pathophysiological models assume that psychosis is caused by hyperactive dopamine (DA) transmission in the mesolimbic pathways and PFC (Brisch, 2014). This is known as the DA hypothesis, and it has been around ever since clinicians have attempted to explain the pathophysiology of psychosis.
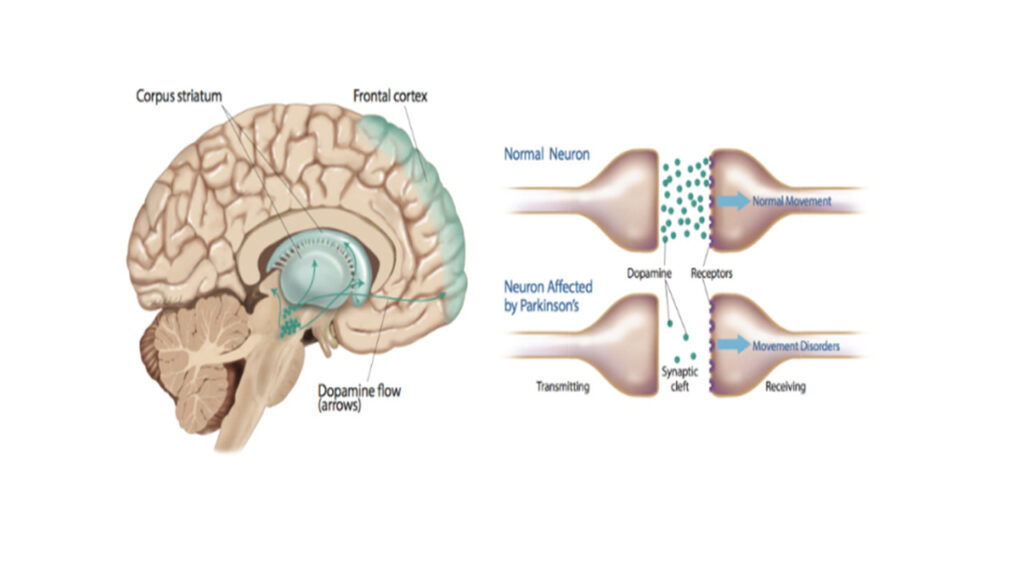 Parkinson’s disease research has majorly contributed in supporting the DA hypothesis. As shown in the above image, Parkinson’s disease is characterized by a significant DA deficiency in the basal ganglia, located in the center of the brain (Brisch, 2014). It is important to note the dopamine theory of schizophrenia has been challenged. Although medications produce their pharmacological effects rapidly, their clinical effects take weeks or months to kick in. This is known as a therapeutic lag. Furthermore, other receptors in other systems are involved along with the dopamine system. Finally, there is a need to reconcile the anatomical/developmental abnormalities.
Parkinson’s disease research has majorly contributed in supporting the DA hypothesis. As shown in the above image, Parkinson’s disease is characterized by a significant DA deficiency in the basal ganglia, located in the center of the brain (Brisch, 2014). It is important to note the dopamine theory of schizophrenia has been challenged. Although medications produce their pharmacological effects rapidly, their clinical effects take weeks or months to kick in. This is known as a therapeutic lag. Furthermore, other receptors in other systems are involved along with the dopamine system. Finally, there is a need to reconcile the anatomical/developmental abnormalities.






